Atherosclerosis
What is Atherosclerosis?
Also known as “hardening of the arteries,” atherosclerosis is a disease in which the arteries are hardened and narrowed as a result of plaque, which has built up along the inside of the artery walls. The disease is a chief contributor to cardiovascular disease, the leading cause of death among men and women in the United States. According to the American Heart Association 2007 Heart and Stroke Statistical Update, atherosclerosis accounts for nearly 75 percent of all deaths from cardiovascular disease.
Millions of Americans have been diagnosed with atherosclerosis, and millions more have the disease but do not know it. Men, African-Americans and all individuals over the age of 65 are especially prone to developing advanced atherosclerosis. In addition, the following factors increase the risk of atherosclerosis, particularly in people with more than one risk factor:
- Diabetes
- Smoking
- Rarely exercising (now considered to be as great a risk factor for heart disease as smoking one pack of cigarettes per day)
- Obesity or being overweight
- High levels of blood lipids (e.g., cholesterol and/or triglycerides)
- Low levels of high-density lipoproteins ("good" cholesterol).
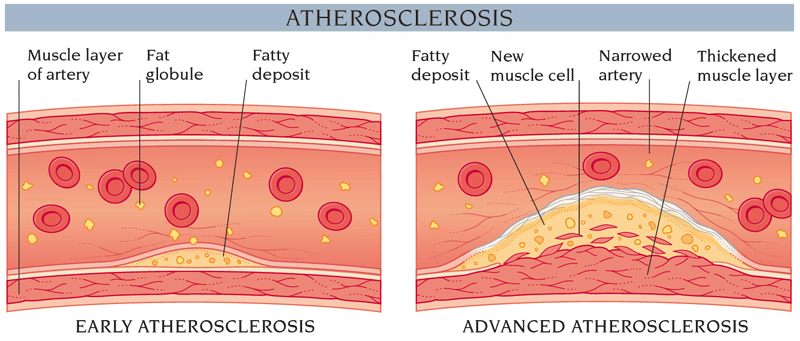 In recent years, scientists have made great strides forward in understanding the atherosclerotic process. The disease tends to be gradual, often taking decades before the affected person is in danger of cardiovascular or cerebrovascular problems. In the early stages of the disease, the inner lining of the artery (endothelium) is damaged. This causes white blood cells to gather at the site of the injury. This in turn provokes an inflammatory immune response that causes further damage to the artery wall. Over time, the endothelium is compromised and large, toxic LDL cholesterol molecules can penetrate into the artery wall. The white blood cells and cholesterol combine to form a lipid foam. In the early stages of atherosclerosis, these fatty streaks are present on the arterial wall as plaque deposits. Fatty streaks have been detected in the arteries of teenagers who were genetically predisposed to develop atherosclerosis.
In recent years, scientists have made great strides forward in understanding the atherosclerotic process. The disease tends to be gradual, often taking decades before the affected person is in danger of cardiovascular or cerebrovascular problems. In the early stages of the disease, the inner lining of the artery (endothelium) is damaged. This causes white blood cells to gather at the site of the injury. This in turn provokes an inflammatory immune response that causes further damage to the artery wall. Over time, the endothelium is compromised and large, toxic LDL cholesterol molecules can penetrate into the artery wall. The white blood cells and cholesterol combine to form a lipid foam. In the early stages of atherosclerosis, these fatty streaks are present on the arterial wall as plaque deposits. Fatty streaks have been detected in the arteries of teenagers who were genetically predisposed to develop atherosclerosis.Over time, the plaque may calcify, or form a hardened "shell." This reduces the supple artery's ability to contract and expand and narrows the artery, thus reducing the amount of blood that can flow through it. A narrowed artery is said to suffer from stenosis, while a completely blocked artery is described as occluded. If the plaque deposit ruptures, a blood clot can form at the site of the rupture, or pieces of the plaque can travel through the arteries until they eventually cause a blockage.
If the affected artery is one of the coronary arteries (located on the surface of the heart), then a lack of oxygen-rich blood to the heart (cardiac ischemia) could cause coronary artery disease (CAD) and, consequently, increase an individual’s risk of the following:
- Angina. A certain type of chest pain, pressure or vague discomfort that indicates an increased risk of a heart attack.
- Heart attack. An event that results in permanent heart damage and can result in death. It is also known as a myocardial infarction, because part of the heart muscle (myocardium) may die (infarction) from lack of oxygen.
- Cardiac arrest. A life-threatening situation in which the heart abruptly stops. The person must be treated with a defibrillator within minutes in order to survive.
- Sudden cardiac death. Death due to cardiac arrest.
Biology of atherosclerosis
A normal artery has many layers. The adventitia is the outermost wall, made up of a fibrous material as well as smooth muscle cells. The media is the central layer of the artery, consisting of multiple layers of smooth muscle cells. The intima is an innermost layer of the artery and is made up of connective tissue, with endothelial cells acting as a lining inside the arteries.
Injury to the endothelial cells is the first step toward atherosclerosis. Researchers have uncovered evidence that atherosclerosis begins with a local injury to the endothelial cells. This injury attracts white blood cells, which provoke a natural inflammatory immune response. Inflammation is central to the healing process. However, in this case, the inflammation occurs in an inappropriate area and tends to further damage the endothelial layer.
In time, the endothelial layer becomes compromised, allowing large, unstable LDL cholesterol molecules to penetrate the endothelium and reach the inner layers of the artery. There, the LDL molecules are exposed to free radicals that are produced as a byproduct of the immune response. This results in the oxidation of the LDL. Oxidized LDL releases a number of toxins into the arterial wall that exacerbates the injury, thus recruiting more white blood cells, which further damage the artery and allow more LDL to penetrate the arterial wall.
Gradually, these substances, including LDL molecules, toxins and white blood cells, form a lipid foam. This lipid foam is the building block of arterial plaque deposits. The foam expands on the arterial wall, slowly growing. Throughout the early stages of this process, the person will likely experience no symptoms.
Once exposed to the circulating blood, the lipid streaks attract minerals such as calcium, which form a hard shell over the plaque deposit. This process is similar to the calcification of plumping pipes, with calcium deposits growing on the inside of arterial walls. In recent years, researchers have made great strides forward in classifying and understanding the nature of the calcified plaque deposits. Deposits covered with a hard, smooth layer of minerals are more stable than those with a soft interior and a brittle and bumpy calcium deposit. A plaque deposit can grown undetected for many years. In fact, some stable plaque deposits can almost totally occlude their artery with no effect. In response to the reduced capacity in that artery, blood is shunted through nearby arteries via collaterals to supply oxygen to the jeopardized heart muscle.
However, plaque deposits that occur in major coronary arteries (e.g., the left main descending coronary artery) or the carotid arteries can pose a significant health hazard. For unknown reasons, a plaque deposit can rupture. When the deposit ruptures, pieces of calcified plaque shower downstream in the artery, where they may become lodged in smaller arteries, thus rapidly blocking blood flow.
Alternatively, circulating blood platelets can detect the site of the rupture and initiate a clotting cascade. In a normal skin injury, this cascade forms a scab, or blood clot. However, when this occurs inside an artery, the result can be the relatively rapid loss of blood flow to organs and tissues beyond the blockage. The result may be a heart attack or stroke.
Risk factors and causes of atherosclerosis
There are many theories about the root cause of atherosclerosis. Studies have shown a genetic component to the disease, and a family history of coronary artery disease is a strong predictor for atherosclerosis.
Other strongly associated risk factors include:
- High blood pressure (hypertension)
- Smoking
- Diabetes
- Advanced age
- Obesity
- Lack of exercise
- Poor diet
A number of emerging risk factors, especially inflammatory markers, have also attracted considerable attention in recent years. Inflammation has been singled out as an underlying factor that both causes and accelerates atherosclerosis. Atherosclerosis itself is an inflammatory process, characterized by activation of the body's inflammatory cascade at the level of the endothelium. This inflammatory cascade is part of a normal immune response. It is thought that atherosclerosis is characterized by a local immune response caused by damage to the arterial wall. As a result, white blood cells gather at the site of the injury and release inflammatory chemicals (such as interleukin-6 [IL-6]) that further damage the arterial wall and attract more white blood cells.
During the atherosclerotic process, the body releases a number of inflammatory markers that can be measured in the blood. These include C-reactive protein, IL-6, lipoprotein-associated phospholipase A2 and others. Currently, only C-reactive protein is regularly used as a marker of heart disease risk, while researchers are examining the role of other inflammatory markers. So far, the data on C-reactive protein has been somewhat mixed. Some studies have found that C-reactive protein is a useful independent measure of heart attack risk, while others have found conflicting results. The source of this conflict might lie in the fact that C-reactive protein is not specific: levels are raised in response to inflammation and injury anywhere in the body. Nevertheless, some physicians recommend monitoring C-reactive protein to measure inflammation in the body.
In the future, lipoprotein-associated phospholipase A2 might emerge as another important tool to measure risk of heart attack. Studies have found that elevated levels of this enzyme are a strong risk factor for heart attack, even in the presence of other normal LDL cholesterol levels.
Another marker of interest is homocysteine. There is considerable debate over the role of homocysteine in heart disease. Homocysteine is an amino acid that is produced as a byproduct of other chemical reactions in the body. High levels of homocysteine may be related to the development of atherosclerosis because it is thought that the amino acid may damage the endothelium and increase the risk of blood clots. Numerous studies have also shown that people with elevated homocysteine are at greater risk for heart attack, stroke and other cardiovascular problems.
However, researchers have been unable to determine if elevated homocysteine levels are caused by heart disease, or if they cause heart disease. Also, two large, well-designed studies have recently shown that moderately lowering homocysteine among people with diabetes and existing heart disease had no effect on lowering risk for cardiovascular events.
At this point, the American Heart Association has not identified elevated homocysteine as a major risk factor for heart disease and does not recommend widespread use of folic acid and vitamin B supplements to lower homocysteine. However, because of the association between homocysteine and heart disease, people are advised to obtain these important nutrients through a healthy diet that includes fruits, vegetables, whole grain and fortified grain products. Additionally, people who have a family history or personal history of heart disease but lack other well-defined risk factors, such as smoking or obesity, should consider monitoring their homocysteine levels.
Signs & symptoms of atherosclerosis
Early atherosclerosis is typically asymptomatic. In later stages, as the arteries become harder and narrower, an individual may start to experience symptoms, depending on the location and severity of the blockage. For instance, pain in the legs (claudication) may signal the presence of peripheral arterial disease, and a certain type of chest pain called angina could indicate coronary artery disease. Carotid artery atherosclerosis rarely has any symptoms, although patients may suffer from transient ischemic attacks, which are a serious warning sign of a major stroke.
Typically, the long-term development of atherosclerosis means that symptoms also develop gradually. However, an occlusion caused by ruptured plaque or a clot could trigger a rapid onset of symptoms.
Diagnosis methods for atherosclerosis
In patients with atherosclerosis, the goal of diagnosis is to determine the location and the extent of the blockage. Atherosclerosis involving the heart and resulting in coronary artery disease may be diagnosed through several tests, including:
Electrocardiogram (EKG)
Following a medical history and physical examination, an EKG is a first-line diagnostic test to detect coronary artery disease. It is a recording of the heart’s electrical activity as a graph on a moving strip of paper or video monitor. The highly sensitive electrocardiograph machine helps detect heart irregularities, disease and damage by measuring the heart’s rhythms and electrical impulses. Easily performed, it can assist a physician in determining if the heart is receiving enough oxygen. The most critical role of an EKG is in patients with acute chest pain to detect a heart attack.
Exercise stress test
If the heart is not receiving sufficient oxygen, the physician will likely want to determine whether exertion aggravates the condition. An exercise stress test is a special type of electrocardiogram that is performed while the patient exercises in a controlled manner on a treadmill or stationary bicycle, at varied speeds and elevations. The reaction of the heart under exertion can be measured and evaluated.
Nuclear stress test
This test involves the administration of a radionuclide substance (e.g., thallium, myoview, sestamibi) into the bloodstream before taking very clear pictures with a gamma camera. Pictures may be taken both at rest and shortly after the stress of exercise. This gives the physician important information about where blockages of arteries may have occurred.
Ultrafast computed tomography (ultrafast CT)
This noninvasive imaging test takes multiple views of the heart. It can measure the amount of calcium in the arteries, which is an excellent indicator of how much calcification has occurred. Because calcified plaque is a sign of atherosclerotic buildup, this test can determine if individuals have an increased risk of coronary artery disease or heart attack regardless of whether symptoms are present. The results of this test are expressed as a calcium score. A low calcium score does not confirm the absence of a blocked artery, and a high calcium score may be associated with a blocked artery. The ultrafast CT is not a substitute for a physician’s evaluation, EKG and exercise stress test.
Where advanced coronary artery disease is suspected, a physician may want to perform a more invasive test called a coronary angiogram. A coronary angiogram is an x-ray of the arteries located on the surface of the heart (coronary arteries). It helps the physician to see if any of those arteries are blocked, usually by fatty plaque. If so, the patient may be diagnosed with coronary artery disease.
To take an angiogram, the physician injects a special dye (contrast medium) into the coronary arteries. To do that, the physician inserts a thin tube (catheter) through a blood vessel, usually in the upper thigh, and guides it all the way up to the heart. Once the catheter is in place, the physician can inject the dye through the catheter and into the coronary arteries. Then the x-ray can be taken. In some cases, blockages can be treated immediately through the catheter while it is still in place.
Treatment options for atherosclerosis
The first goal for treatment of atherosclerosis is to restore as much blood flow as possible through the affected portion of the vascular system and to reduce the risk of a plaque rupture, which can result in a heart attack or stroke. This can sometimes be achieved by reducing risk factors, getting regular exercise and/or taking medications such as:
- Antiplatelets (e.g., aspirin) inhibit the formation of blood clots by decreasing the ability of platelets (the body’s natural blood-clotters) to bind together. In the case of atherosclerosis, antiplatelets prevent a damaged vessel from becoming blocked due to excessive concentration of platelets.
- Beta blockers reduce the workload of the heart by blocking the effect of adrenaline and the sympathetic nervous system on the heart.
- Nitrates work directly on blood vessels supplying the heart muscle, causing them to relax and allowing oxygen-rich blood to reach the heart.
- Cholesterol-reducing drugs (e.g., statins) lower the patient’s level of fats (lipids) in the blood, such as cholesterol and triglycerides. High LDL levels are associated with increased risk of heart attack and stroke.
- ACE inhibitors block the production of a substance that causes blood vessels to tighten, allowing more oxygen-rich blood to flow into the heart.
- Vitamins may also be helpful, especially folic acid, which counteracts the dangerous effects of certain amino acids. Folic acid should always be taken in conjunction with vitamin B12 because folic acid can mask a vitamin B12 deficiency. However, it should only be administered as directed by a physician.
Balloon angioplasty
A balloon-tipped catheter presses plaque back against the artery walls, increasing the amount of room through which blood can pass through the vessel.
Stenting
A wire mesh metal tube called a stent can be inserted into the area of a damaged artery. The stent acts as a scaffold, stretching and supporting the artery walls, and permitting blood to flow freely through the previously blocked vessel. Newer stents are coated with special drugs that help prevent restenosis, or reclosure of the artery after the procedure.
Atherectomy
A procedure that uses a specialized catheter that removes plaque by cutting or grinding it away. Depending on the technique used, the residue is pulverized and 1) allowed to flow harmlessly through the bloodstream; 2) removed as the catheter is withdrawn; or 3) vacuumed through the catheter and out of the body during the procedure.
With severe disease, or atherosclerosis that occurs in multiple veins or coronary arteries, a coronary artery bypass graft (CABG) may be recommended. During this form of open-heart surgery, a heart surgeon uses vein grafts to bypass the blocked portions of the coronary arteries. In the carotid arteries, severe disease may be treated with a procedure called a carotid endarterectomy. During this procedure, the surgeon exposes the arteries in the neck, then strips away the inner lining of the artery, including the plaque deposit.
Prevention methods for atherosclerosis
The first-line defense against atherosclerosis is to limit the damage caused by the disease and prevent it from worsening. To do this, physicians will often recommend the following strategies:
Quitting smoking
Tobacco smoking is a major cause of coronary artery disease (CAD) and cardiac arrest. Research from the Centers for Disease Control and Prevention (CDC) shows heart disease as the leading smoking-related cause of death in the United States among men and women, resulting in about 150,000 deaths from cardiovascular disease each year. The average smoker dies nearly seven years earlier than a nonsmoker, according to the CDC.
Controlling diabetes
Persons with diabetes may be more likely to develop heart-related diseases, and diabetes is associated with more severe atherosclerosis. Proper glucose control is crucial to the overall health and heart function of diabetic patients.
Controlling high blood pressure (hypertension)
Individuals with high blood pressure are at greater risk of cardiovascular problems resulting from CAD. Hypertension can be controlled through taking blood pressure medications (antihypertensives), self-monitoring blood pressure, eating a heart-healthy diet that is low in salt and engaging in regular exercise. People are also encouraged to have regular check–ups with their physician.
Fats and cholesterol
Reducing the amount of fats and cholesterol in one’s diet to lower total cholesterol levels. High cholesterol levels are not thought to cause atherosclerosis directly. However, cholesterol is thought to trigger other abnormalities that may speed the process of plaque build-up.
Achieving and maintaining a healthy weight
Obesity and being overweight are major risk factors for a host of serious health conditions, including coronary artery disease, high blood pressure, diabetes, heart attack and stroke. Some weight control methods include limiting unhealthy fats (e.g, saturated and trans fats) in a patient’s diet, increasing activity levels, counseling, medication and surgical interventions.
Exercise
Keeping a routine of moderate to vigorous exercise, depending on an individual’s overall health. This is valuable in maintaining a healthy cardiovascular system. Exercise keeps obesity at bay and keeps the heart from being unduly stressed. It also lowers cholesterol levels and blood pressure. Furthermore, when accompanied by a low-fat diet, exercise may help to reduce plaque deposits, reversing the process of atherosclerosis. Current guidelines recommend 30 minutes of exercise most days of the week.
Learn your family medical history
A patient’s family medical history can greatly increase (or decrease) the risk of the patient developing certain medical conditions, including atherosclerosis and coronary artery disease. Some patients prefer to develop their own medical family tree and bring it with them to their medical appointment. A complete family tree traces the medical history of an individual (and spouse, if applicable) through at least two generations.
Physical examinations
Getting regular physical examinations, particularly if in a high-risk category for heart disease.
Stress management
Stress can lead to high-risk practices such as overeating, smoking, high blood pressure (hypertension) and a lack of exercise. In addition, chronic stress may be a direct contributor to poor heart health because it produces increases in blood pressure that could become permanent.
Controlling chronic depression
Depression has been linked with a higher risk of developing high blood pressure, heart disease and having a heart attack.
Until recently, high estrogen levels had been believed to provide younger women a significant degree of protection from the development of heart disease in their premenopausal years. Indeed, earlier studies investigated a role for hormone replacement therapy (HRT) in continuing this protection in postmenopausal women.
However, a major study of cardiovascular protective effects of estrogen-progesterone HRT, called the Women’s Health Initiative, yielded unexpected results. Researchers found that HRT consisting of estrogen and progesterone increased the risks of heart attack, breast cancer, blood clots and overall cardiovascular disease. A second portion of the same study found that estrogen-only HRT also raises the risk of heart disease. Neither form of HRT is recommended for the primary prevention of heart disease, although they might still be recommended for prevention of osteoporosis or to prevent the symptoms of menopause. Research is ongoing into the benefits and risks of low-dose HRT.
Questions for your doctor about atherosclerosis
Preparing questions in advance can help patients have more meaningful discussions with their physicians regarding their conditions. Patients may wish to ask their doctor the following questions about atherosclerosis:
- Can my atherosclerosis be healed or reversed?
- Does having atherosclerosis mean I'm definitely going to have a heart attack or stroke?
- What are the most important things I can do to help my own prognosis?
- If I have been having hormone replacement therapy, should I stop?
- Should my children be checked for developing atherosclerosis?
- If we treat one area, what are the chances that the disease is affecting other organs?
- How can I tell if the disease is in other arteries?
- What other risk factors for a heart attack do I have that should be controlled?
- How can we measure my progress?
- Are there any dietary nutrients and supplements I should take? Are there any I should avoid?
- How long will I be taking the prescribed medications?
Additional Information
Medications
- Since the damage has already been done, there is no satisfactory medicine that can treat atherosclerosis.
- Recent studies show that lowering cholesterol levels in persons with high levels can increase life expectancy. If you have symptoms of a disorder caused by atherosclerosis and diet and exercise fail to reduce cholesterol, antihyperlipidemic drugs may be prescribed.
- Other drugs may be necessary to treat symptoms of an associated problem (high blood pressure, heartbeat irregularities).
- Some studies have indicated that aspirin and vitamin E may reduce the risk of heart attack. Get medical advice to see if they should be recommended for you.


Activity
- Usually no restrictions. Activity will depend on general state of health and any other illnesses present.
- A routine exercise program is encouraged.
Diet
Eat a diet that is low in fat and low in salt and high in fiber. Increase your intake of grains, fresh fruits and vegetables.
What might complicate it?
- Heart attack.
- Stroke.
- Angina pectoris.
- Kidney disease.
- Congestive heart failure.
- Heartbeat irregularity problems.
- Sudden death.
Predicted outcome
Asymptomatic disease usually does not result in disability. However, symptoms may eventually develop, depending on the extent to which risk factors can be modified. In symptomatic disease, the prognosis depends on the specific diagnosis such as coronary, cerebrovascular, or peripheral vascular disease, or aortic aneurysm, the severity and extent of disease, the type of treatment, response to treatment, the presence or absence of complications, and the modification of risk factors.
Appropriate specialists
Internist, cardiologist, cardiovascular surgeon, neurologist, and vascular surgeon.
Notify your physician if
You or a family member has high risk factors for atherosclerosis and want to become involved in a prevention program.
